- Maximize Your Practice Revenue
AI Agents for Medical Billing Automation
MedSky Billing steps into the future of RCM automation with intelligent AI agents. They handle prior authorizations, denials, and other repetitive billing tasks, driving up collections by 20%.
Get Free Consultation
- AI-Powered Claim Submissions
- Minimal Errors
- Maximum Reimbursements
AGENTS
Which AI Agents Has MedSky Built to Automate Every Step of RCM?
ELIXA
This AI agent instantly verifies patient eligibility and insurance coverage in real time, eliminating manual checks. It reduces claim rejections and ensures every claim is submitted with accurate patient data.
PRIA
It accelerates prior-authorization approvals by automating submissions and payer follow-ups. This automation tool minimizes delay and facilitates faster patient care through its authorization tracking.
CODIN
Our team uses this AI agent to ensure coding accuracy using AI-driven algorithms and compliance rules. It uses up-to-date CPT/ICD-10 usage and optimizes payments through precise code selection.
CLAIR
MedSky has built this RCM automation tool to handle claim scrubbing, creation, and submission. This AI agent detects errors before submission and delivers cleaner claims for faster reimbursements.
DEXA
With this billing AI agent, identify denial trends, automate appeal generation, and prevent repeat denials. It learns from past payer responses to improve future claim success rates and revenue recovery.
ARIS
Using this AI healthcare solution, automate A/R follow-up communication with payers to handle claims. This AI RCM agent shortens payment cycles and prevents revenue leakage effortlessly.
REMITA
This AI agent automates payment posting, reconciles remittances, and detects discrepancies instantly. With this medical billing automation tool, you can get real-time financial visibility for your practice.

Why Do Practices Need AI RCM Agents to Automate Billing?
Healthcare professionals need an automated billing system to bypass manual tasks and delayed payments. Here is why you need our AI agents:
Claim Denials and Rejections
Up to 30% of claims face denial due to manual errors. AI agents provide real-time verification and clean submissions for faster collection.
Time-Consuming Prior Authorizations
Staff spend over 14 hours weekly on authorizations. Automation will cut approval times by 60% and improve patient satisfaction.
Coding Errors and Compliance Issues
Manual coding causes 63% of denials. With AI agents, we assign accurate CPT codes, improving coding precision by 99%.
Inefficient Denial Management
Practices recover only 70% of denials. RCM automation helps in denial tracking and appeals, helping recover lost revenue.
CONTACT US
Tired of Denials and Delays? Let Our AI Agents Handle Billing for Your Practice.
How MedSky AI Agents Can Help You Automate Medical Billing?
ELIXA – AI Eligibility Verification Agent
ELIXA transforms eligibility verification with intelligent medical billing automation. It connects to EHRs and payer systems via EDI, APIs, and AI-driven calls to interpret coverage data in real time. It even shows the number of eligibility checks that required prior authorization. On its dashboard, you can see Live AI Activity to analyze the eligibility verification status happening through billing automation. It even tracks claim details and verification trends.
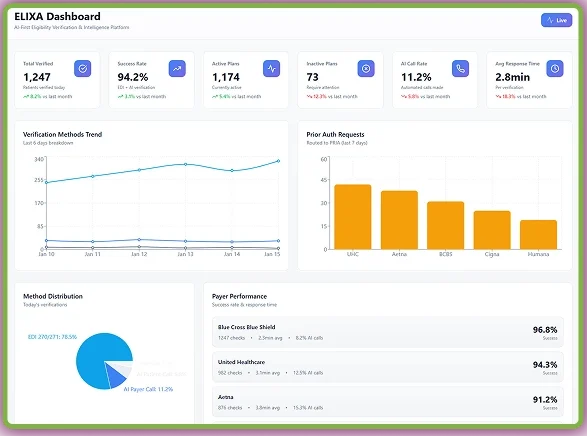
PRIA – Prior Authorization AI Agent
PRIA automates case detection and payer follow-ups with over 97% accuracy. Its Predictive Risk Heatmaps identify high-risk denials before they happen. Moreover, the AI Call Center automates payer calls to drastically reduce manual phone time spent on getting status updates or submitting verbal PAs. Within the dashboard, you can track integration performance with different payer portals. This agent gives AI confidence in its decision to show it has selected the correct payer.
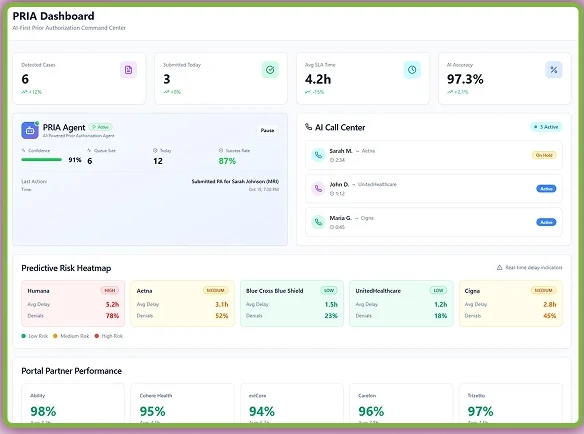
CODIN – AI Coding and Compliance Agent
CODIN automates medical coding with AI that reads clinical notes, extracts diagnoses, and procedures. After extracting data points with its OCR technology, matches them to the correct CPT and ICD codes. It audits every claim, detecting NCCI or MUE violations and flagging missing documentation.
Moreover, this medical billing automation agent analyzes prepared claims to suggest the right codes for higher reimbursements.
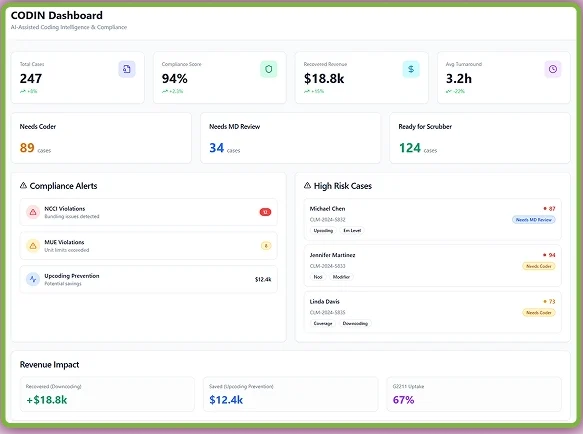
CLAIR – AI Claim Scrubbing and Creation Agent
CLAIR is your intelligent claim scrubbing AI agent designed to eliminate denials before they happen. It analyzes claim line items (codes, modifiers, coverage, provider info) using AI and payer rules. The dashboard even displays live clean rates, denial trends, and system accuracy. Surprisingly, this AI agent auto-fixes minor issues like modifier errors or code mismatches using trained models. Moreover, it compares each claim against historical denial patterns.
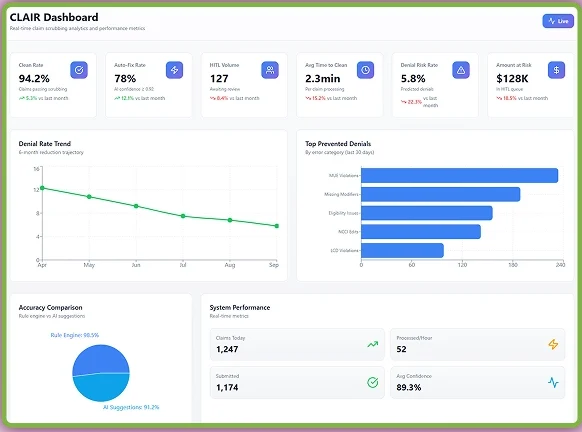
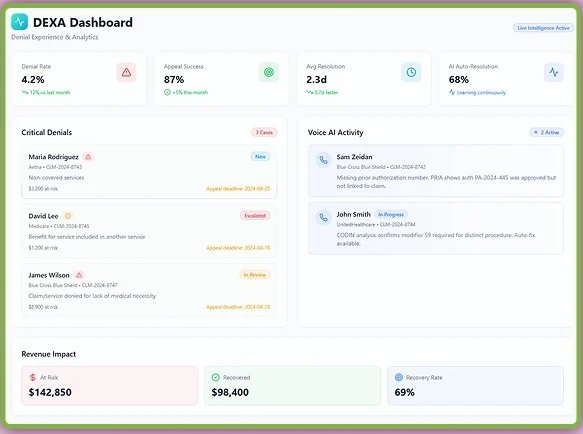
DEXA - Denial Experience and Analytics Agent
DEXA revolutionizes denial management by turning payer rejections into revenue opportunities. This AI agent detects, analyzes, and resolves denials in real time. DEXA documents each call outcome in real time and updates claim statuses automatically in the EHR or billing software. More importantly, this AI RCM tool auto-categorizes critical denials, generates appeal letters, and even calls payers to verify claim details.
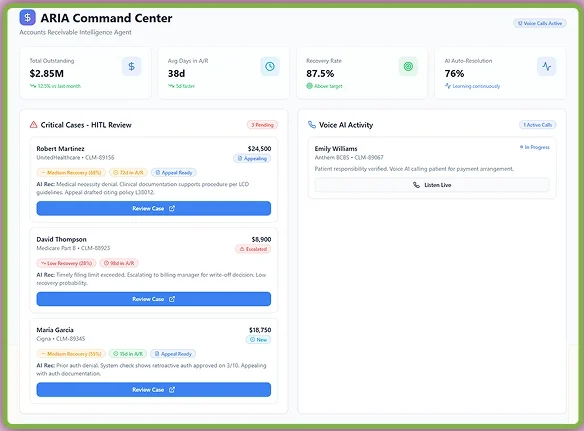
ARIS - Accounts Receivable Intelligent System
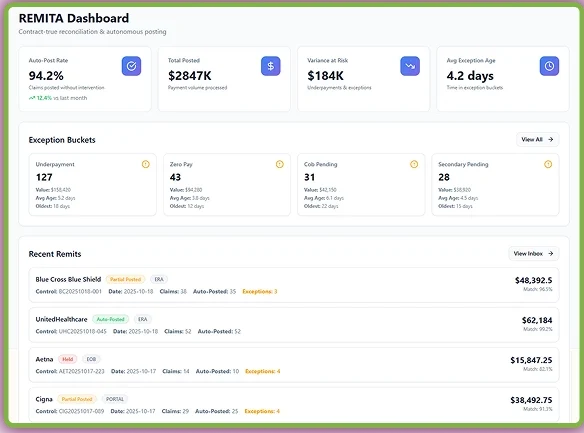
REMITA – Reconciliation and Autonomous Posting Agent
REMITA is an AI automation tool for payment reconciliation and exception management in the healthcare RCM. This AI billing agent auto-reconciles remittance data (ERAs and EOBs) with expected payments and posts payments automatically to patient and insurance accounts. Plus, this agent detects and flags exceptions, such as underpayments, denials, or missing info. Overall, it reduces manual intervention by continuously learning payer patterns.
WHY CHOOSE US
Why Should You Choose MedSky AI RCM Agents for Billing Automation?
Near-Perfect Claim Accuracy
Your practice can achieve around 99.99% claim accuracy after completely adopting all of these AI agents into your workflow. Our AI claim scrubbing detects coding, modifier, and NCCI errors before claim submission.
Faster Eligibility Verification
Our ELIXA AI Agent for Medical Billing verifies patient eligibility in just 4 seconds, replacing weeks of manual work. It accelerates front-end billing, reduces claim delays, and empowers your team to deliver more efficient patient care.
Cost and Time Savings
By automating verification, coding, claim scrubbing, and payment posting, MedSky’s AI agents reduce manual effort by up to 70%. In this way, you can save resources and money required to be spent on the human workforce.
Auto-Resolution of Claims
With the involvement of advanced AI, agents like DEXA and ARIS do their job to resolve every stuck claim automatically. You can expect an auto-resolution rate of over 80%, without needing any human intervention.
Revenue Improvement
After fully implementing AI agents for medical billing automation, you can see improvements in collections. Most of our clients see revenue growth of around 10 to 15% within a few months of automating the billing cycle of their practice.
Real-Time Financial Visibility
On our main dashboard, you will get insights about eligibility scores, revenue collected, appeal success, and many other factors. Practices gain financial insights and monitor areas of concern through the module health dashboard.
What You Can Achieve Through Our AI Agents for Medical Billing?
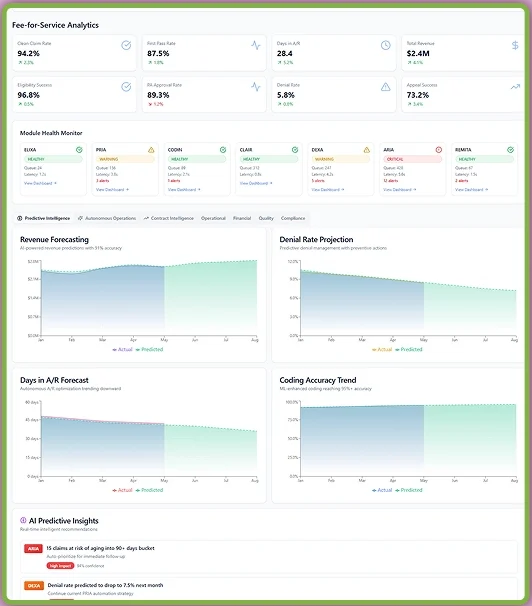
Actionable Insights from Your AI RCM Agents
Our Master Command Dashboard gives you a data-driven view of how these AI agents are performing across every stage of the revenue cycle. You get the following insights:
Predictive Analytics
Our AI predicts revenue trends, denial spikes, and coding accuracy so you can act early and strengthen financial performance.
Performance Tracking
Using this dashboard, track first-pass rates, collections, and A/R days to measure automation success and maximize profitability.
Health Monitoring
Instantly spot which RCM modules excel and which need tuning to make sure that your AI agents run at peak efficiency every day.
AI Predictive Insights
You will get AI-powered alerts on denials, delays, or underpayments before they impact revenue, so your team stays financially confident.
Testimonials
What Our Clients Say
Trusted by 300+ Verified Practices
I would like to send out a heartfelt appreciation for all of your hard work in helping my Health Counselling clinic take care of our billing and credentialing needs. You have made my job as a practice owner much easier.
FAQS
Frequently Asked Questions
In 2025, eligible clinicians get to choose and report out of 199 MIPS Quality measures. These measures are available through a range of collection types, one of which is a MIPS registry. As a MIPS consultant, it is on us to report most efficiently for you to score high and handsome. In short, it is a burden-free MIPS data submission method leveraging ease, peace of mind, and incentives at the same time.
In 2022, while we submit your data before the deadline, you can expect up to 5% incentives with MedSky Billing Solutions.
Because it is hassle-free. You don’t have to take the burden of reporting, instead, it is the registry that takes the stress on your behalf. CMS-recognized registries establish, verify, and validate data as per the requirements of your specialty or practice.
First, your eligibility has to confirm. Second, you have to share your input in selecting measures. MIPS full form in healthcare returns profits on your Medicare reimbursement resulting in increased revenue. Give us a call; we won’t take much of your time and get right to it.
Not at all. It’s pretty easy on the pocket. However, it is not a one-size-fits-all thing with the pricing. Since your practice may have more than one clinician who has to report MIPS, prices vary. Besides, they also vary from specialty to specialty. Therefore, it is best to leave your info such as NPI, the best time to call, whom to talk to at info@medskybilling.com; and, we’ll try to back to you as soon as we can.
