Manage Payer Contracts - Credentialing AI
- 1500+ Satisfied Providers
- Serving More Than 75 Specialties
- 1200+ Billing and Coding Experts
We are integration specialists



Advanced Credentialing AI Solutions
Payer Benchmarking
Compare your contracted rates against local and national standards.
Centralized Contract Management
All your payer contracts, terms, and fee schedules in one secure dashboard.
Rate Modeling
Simulate negotiation scenarios to understand the financial impact before you sign.
Automated Underpayment Detection
Continuously scan payments to identify when payers reimburse below contracted rates.
Recovery Workflow Tools
Automated tasks to track and claim every dollar you are owed.
Data Reporting and Export
Generate powerful reports to drive negotiations and recoveries.
Are You Ready To Recover Your Revenue Swiftly?
Credentialing AI enhances and simplifies the management of payer contracts, offering robust benchmarking and automating the detection of underpayments to facilitate quick revenue recovery.
Why Our Credentialing AI?
The Old Way
Siloed Payer Contracts
Lack of Rate Benchmarking
Undetected Underpayments
The Medientsky AI Way
Streamlined Contract Management
Benchmarking Capabilities
Automated Underpayment Detection
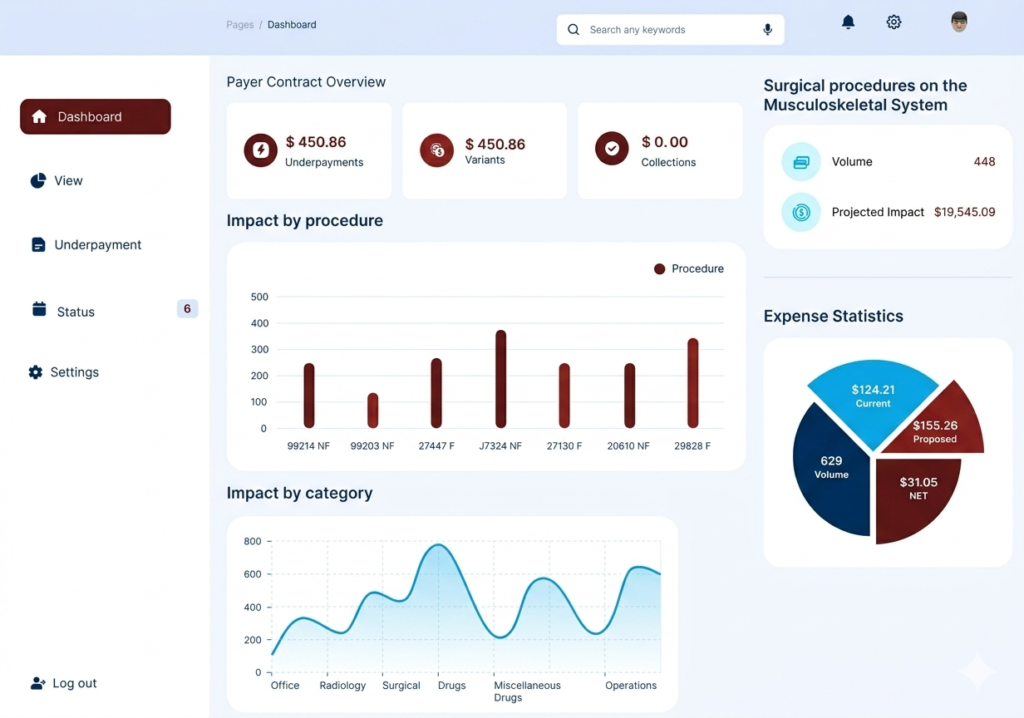
Credentialing AI - Dashboard Feature Overview
Benchmarking overview
Multi-Level Rate Benchmarking
Compare your reimbursement rates against local, state, or national averages.
Payer Relationship Health
Real-time insights into the status and performance of your payer partnerships.
Export-Ready Reports
Generate professional reports to share easily with payer representatives.
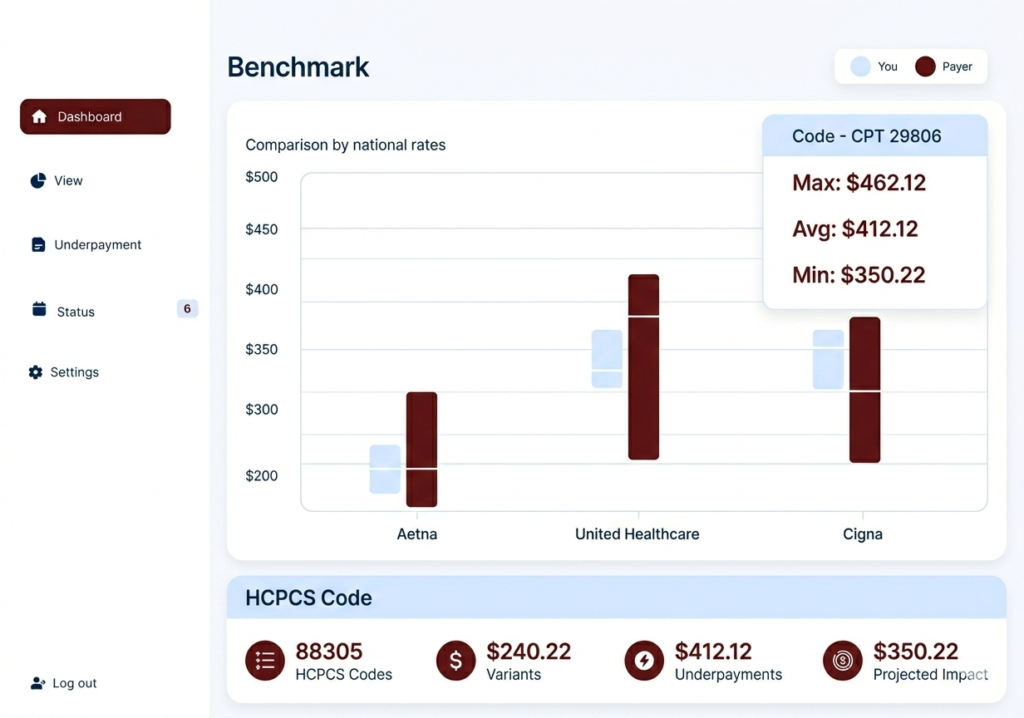
Payer contract overview
Intelligent Contract Guidance
Enhance negotiations with data-driven insights showing the probability of proposed changes.
Scenario Simulation
Model potential financial outcomes to maximize performance before signing.
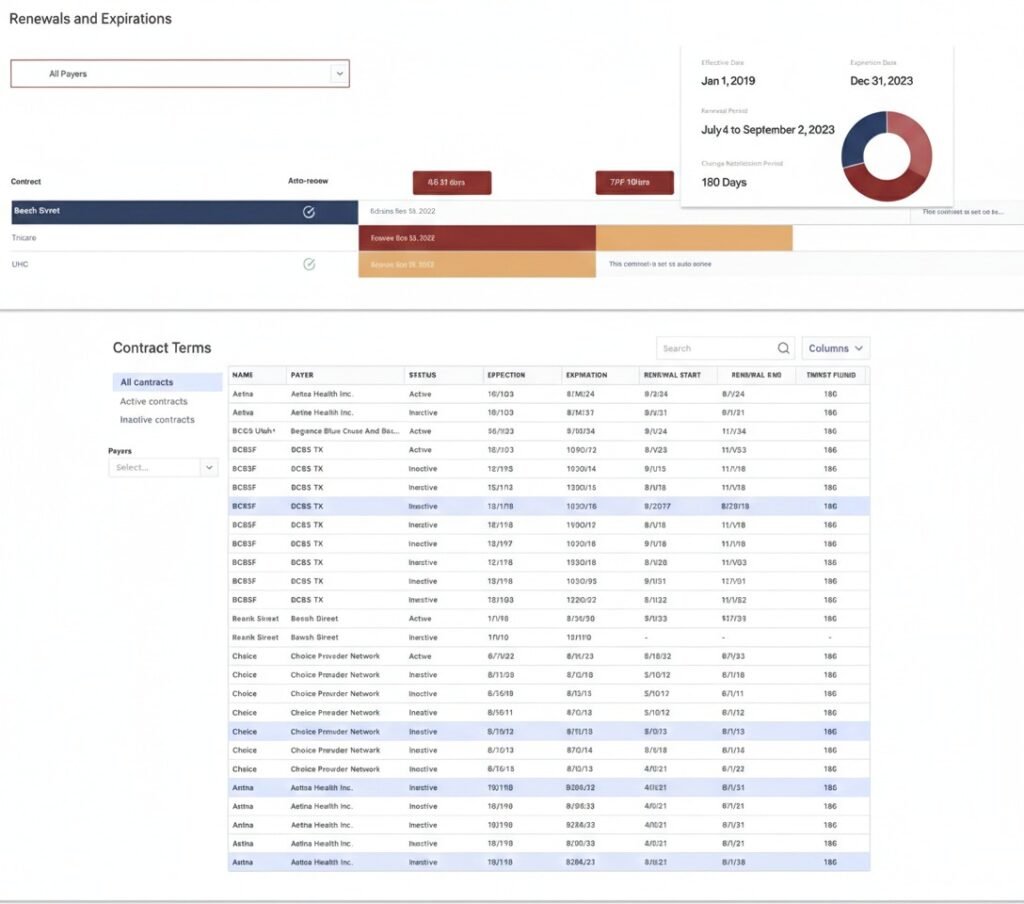
Contracted rate overview
Short-Payment Analysis
Automated audits to identify recurring reasons for underpayments.
Systemic Variance Detection
Pinpoint patterns and trends to prevent issues at scale.
Instant Downcoding Audit
Real-time payer audit to flag and challenge inappropriate downcoding.
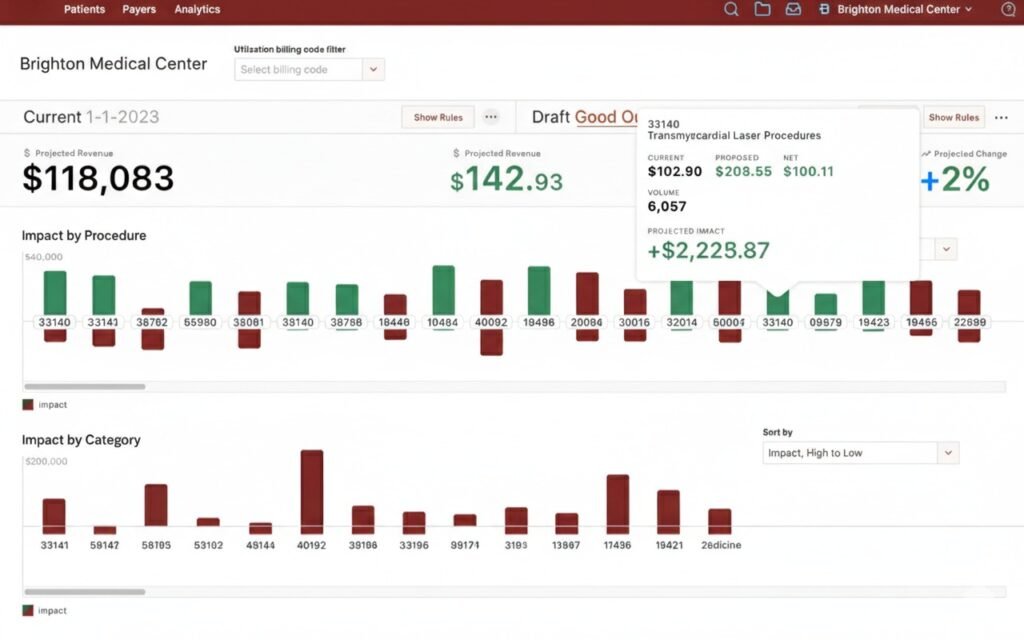
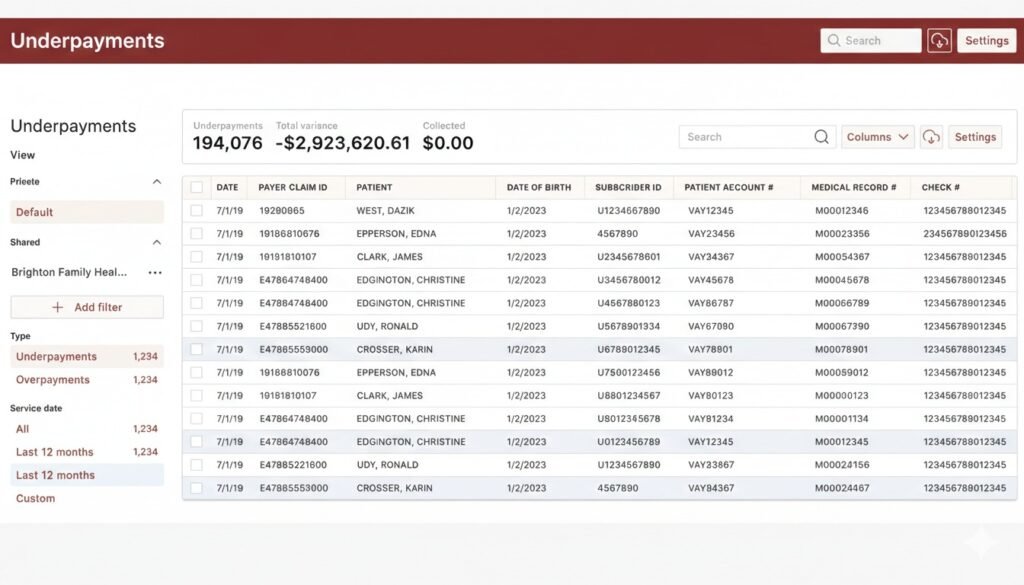
Underpayment detection
Appeal Project Tracking
Highlights underpayment projects and appeal types to ensure accurate reimbursement.
Comprehensive Documentation
Maintain regular records for seamless tracking, reprocessing, and resubmission.
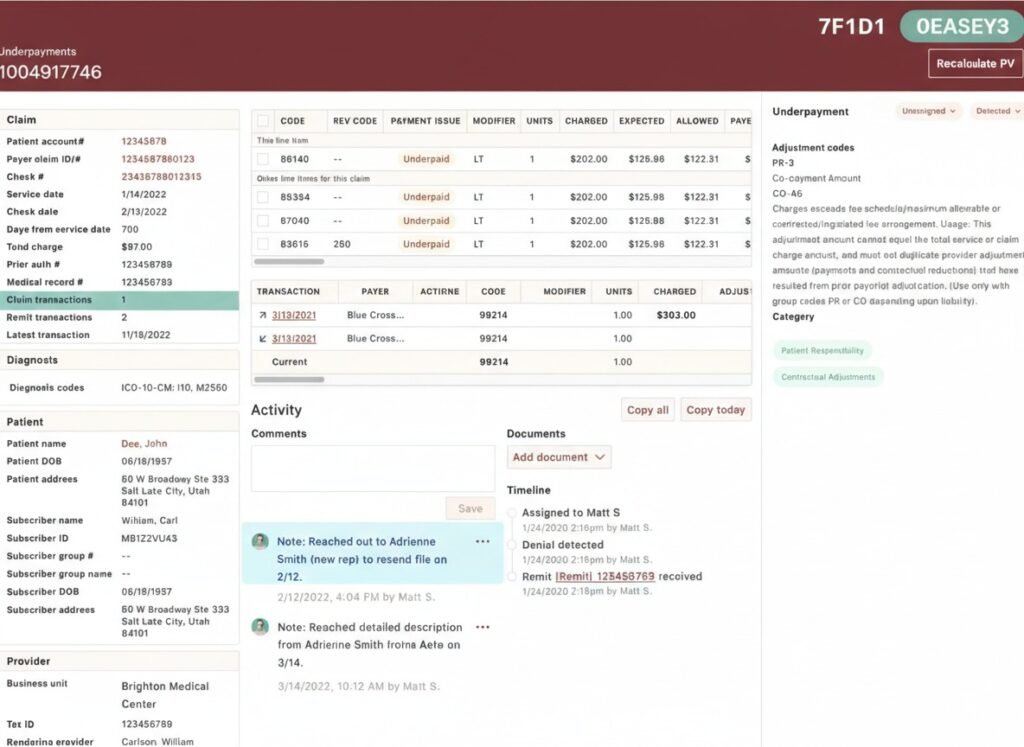
Reimbursement recovery
Centralized Rate Access
View all your contracted rates in one secure location.
Intuitive Dashboard
User-friendly interface for quick and easy rate management.
Rate Comparison Tool
Instant lookup to compare current rates against reduced fee schedules.
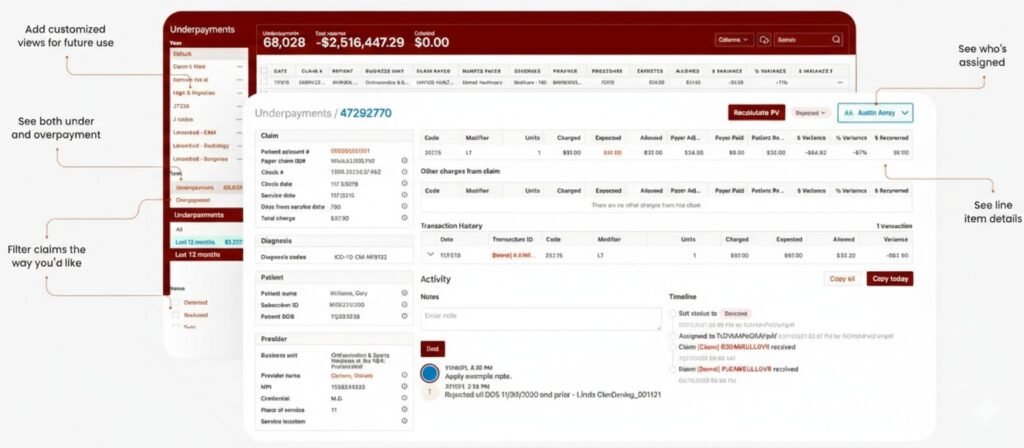
Negotiate Payer Contracts Right
Testimonials
What Our Clients Say
Trusted by 300+ Verified Practices
I would like to send out a heartfelt appreciation for all of your hard work in helping my Health Counselling clinic take care of our billing and credentialing needs. You have made my job as a practice owner much easier.
Understaffed Payer Contract Management Team?
Let our team handle the complexity. We ensure that providers meet payer requirements in a timely manner and remain informed about recredentialing deadlines. We focus on streamlining credentialing workflows, managing documentation, and coordinating with payers to minimize delays, which helps reduce denials related to credentialing problems. Additionally, we utilize data and automation to monitor credentialing statuses, pinpoint potential gaps, and ensure compliance, ultimately facilitating quicker reimbursement for your practice.
