The Smarter Way to Protect Your Revenue
Introducing DenialAI by Medientsky Billing—the intelligent denial management system that predicts, prevents, and resolves claim denials before they hit your bottom line. Powered by machine learning, DenialAI analyzes denial patterns, automates appeals, and gives you back the time you spend chasing payments.
- 1500+ Satisfied Providers
- Serving More Than 75 Specialties
- 1200+ Billing and Coding Experts
We are integration specialists



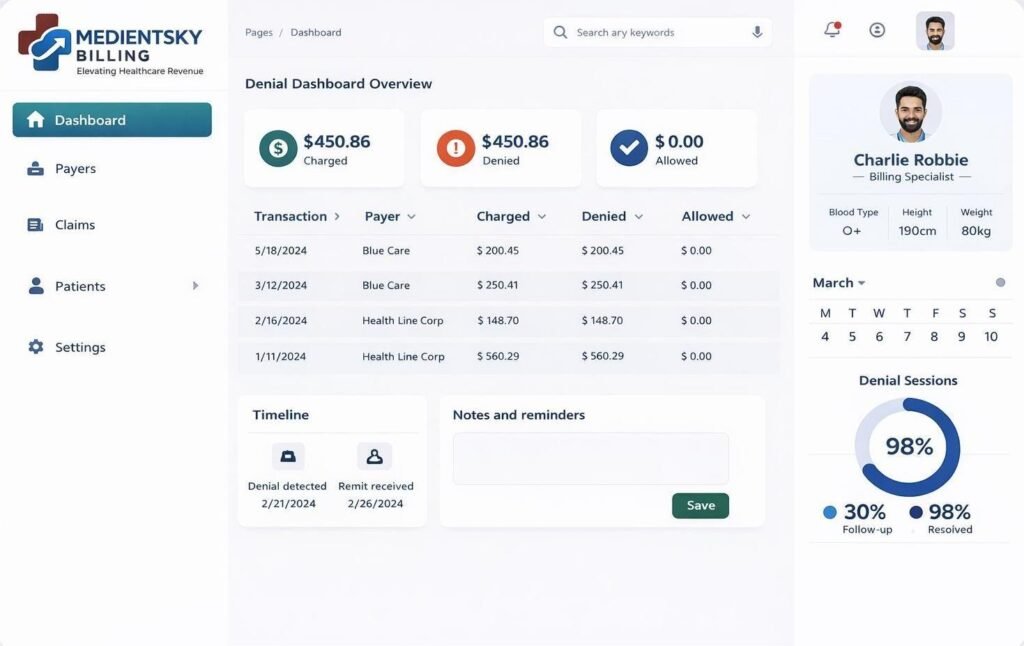
DenialAI: Your 24/7 Revenue Protector
Predict & Prevent
Stop denials before they happen.
Automate Appeals
Resubmit denied claims faster.
Recover Revenue
Turn lost income into collected cash.
Did you know?
The Cost of Denials is Too High to Ignore
The average healthcare provider loses nearly 5% of their net revenue to claim denials, and 65% of denied claims are never resubmitted.
Eligibility Errors
Missing or incorrect patient coverage details.
Coding Mismatches
ICD-10 codes that don't support the CPT procedure.
Authorization Gaps
Missing prior authorizations for services rendered.
Timely Filing Lapses
Resubmissions that miss critical deadlines.
DenialAI eliminates these gaps.
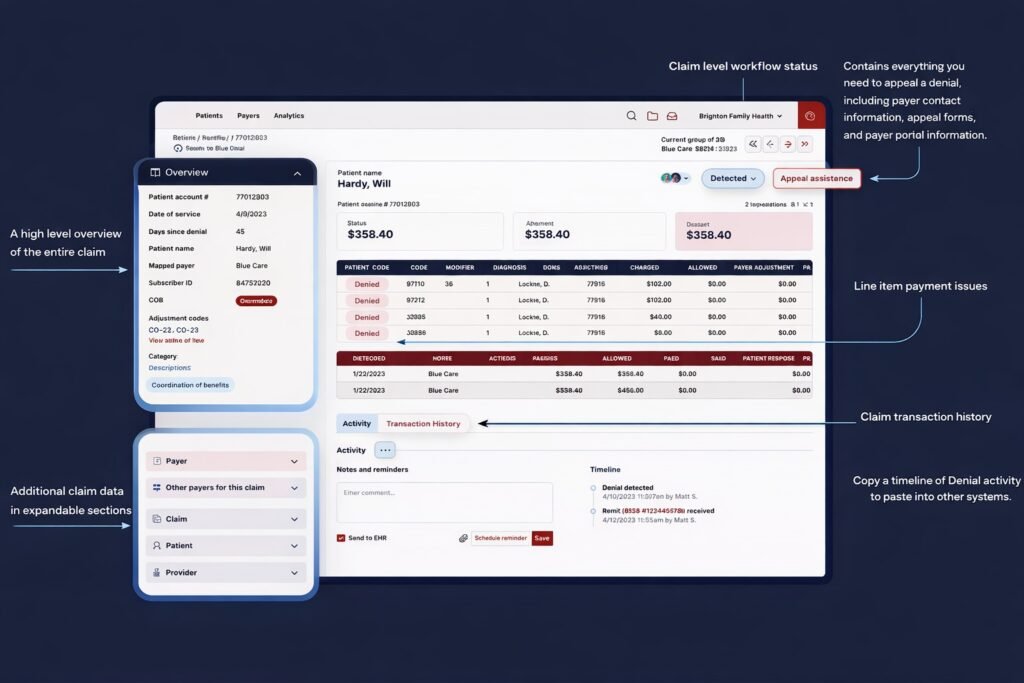
How DenialAI Transforms Your Workflow
Intelligent Risk Scoring
Root Cause Analysis
Automated Appeal Generation
Real-Time Visibility Dashboard
DenialAI Feature Deep Dive
Revenue Recovery
Clear Denial Lists
Easy-to-read inventories of all denied claims.
Comprehensive Status Views
Both high-level overviews and detailed insights into every claim.
Customized Worklists
Tailored lists designed to streamline your denial resolution process.
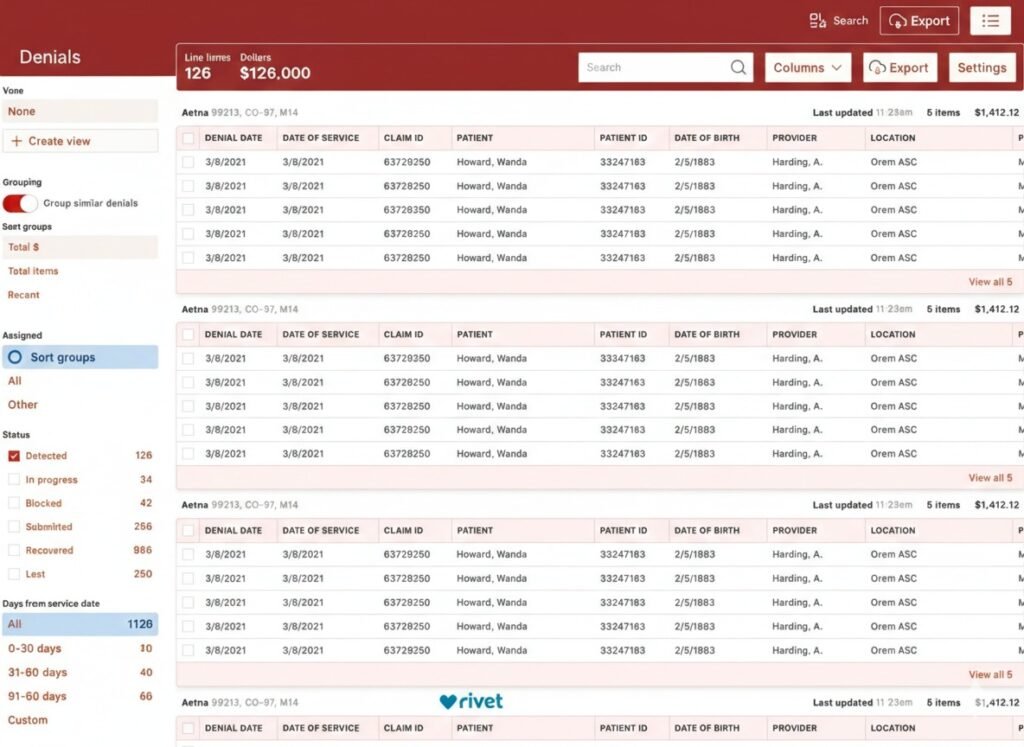
Expandable denial lengths
Quick Filters for Batch Processing
Efficiently filter and process claims in batches to save time.
Prioritized Worklists
Organized lists designed to help your team focus on what matters most.
RCM Knowledge Guides
Flexible resources to expand your team's revenue cycle management expertise.
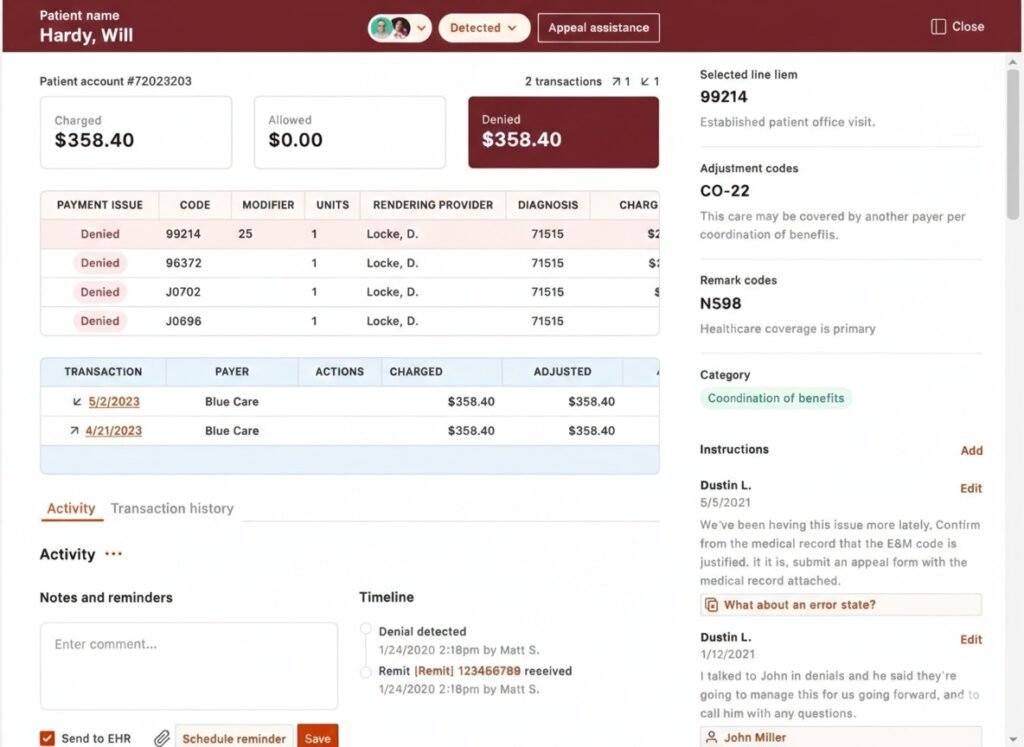
Faster appeals
Accelerated Form Filling
Browser plugin automatically populates online forms to save valuable time.
Deadline-Driven Alert
Smart notifications help your team prioritize work based on critical filing deadlines.
Batch Appeal Exports
Easily export appeals in bulk to share efficiently with payer representatives.
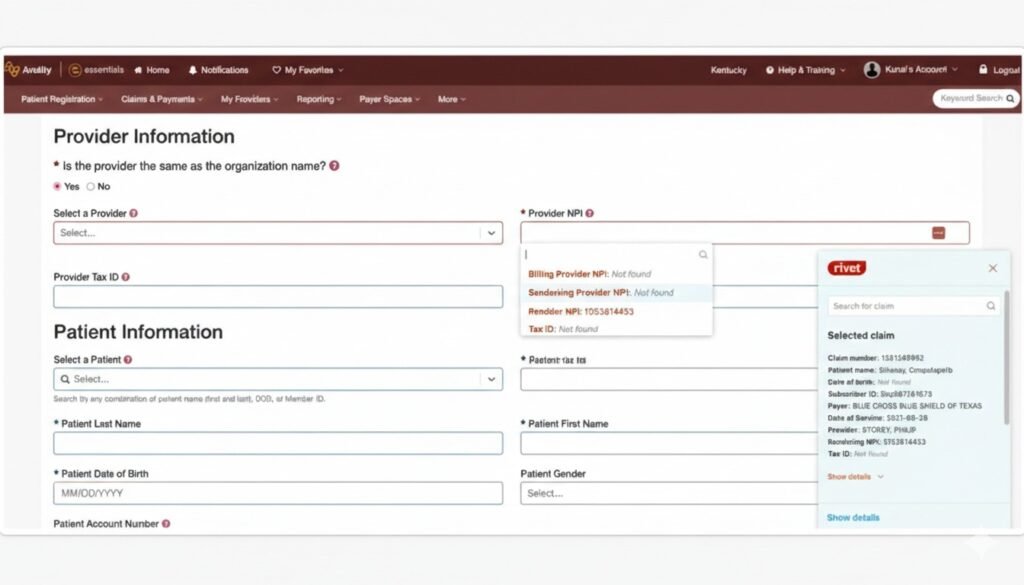
Improved productivity
Live Progress Updates
Real-time visibility into team performance to boost motivation and accountability.
Multi-Level Recovery Views
Customized data dashboards for both managers and individual team members.
Trackable Submission Metrics
Monitor key data points to ensure faster, more efficient claim submissions.
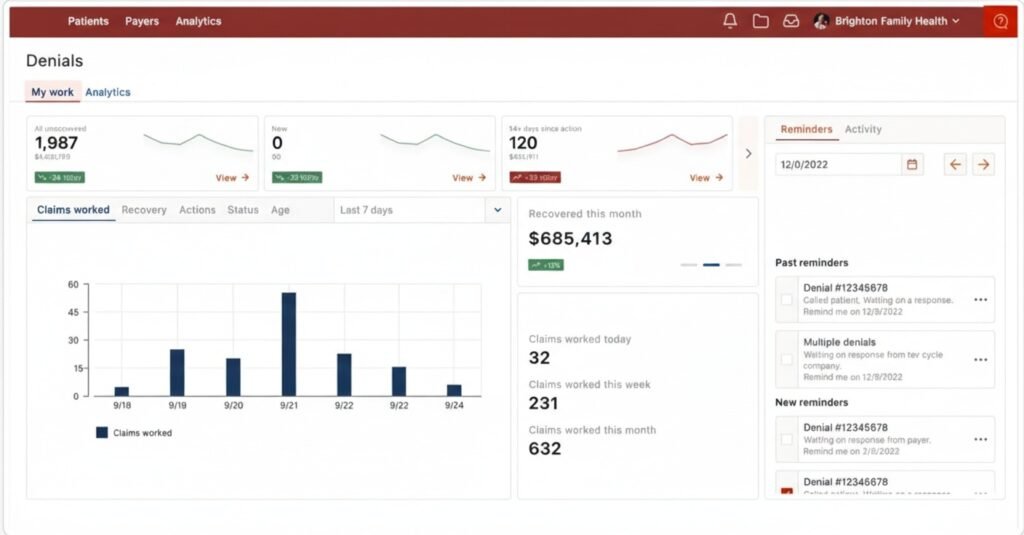
Analytics
Root Cause Analysis
Identify the main causes of denials to prevent recurrence.
Benchmark Comparison
Compare your denial rates against industry standards.
Automated Overdue Checks
Systematic alerts for claims approaching or exceeding timely filing limits.
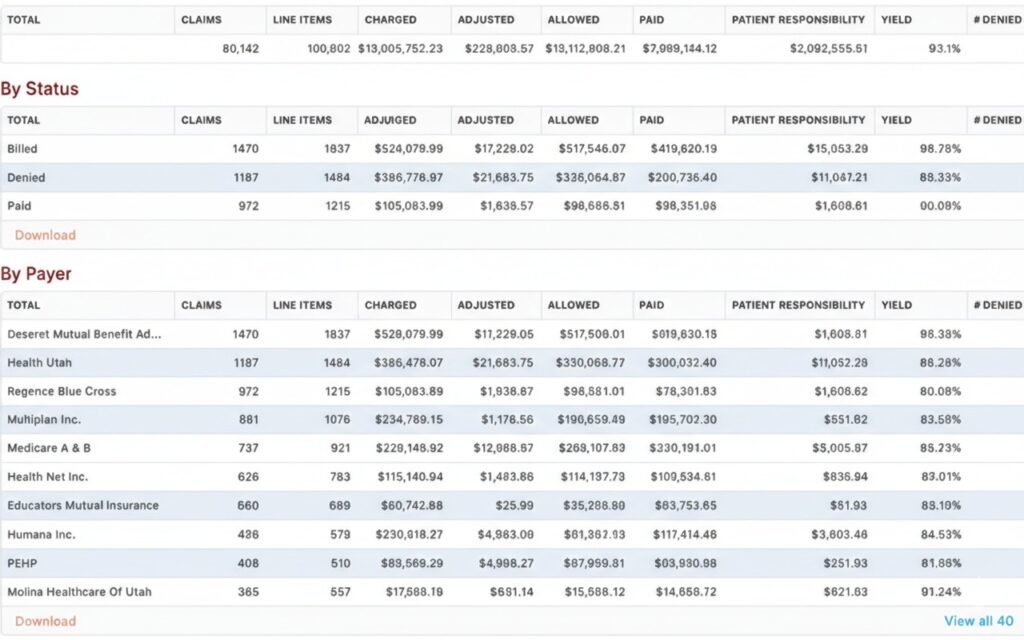
Don't Just Fix Denials also eliminate Them
The average practice spends 20+ hours a week managing denials. That’s time, money, and resources wasted.
- With Medientsky DenialAI, you can:
- Reduce your denial rate by up to 40% .
- Cut appeal resolution time in half .
- Increase your team's productivity by 30% .
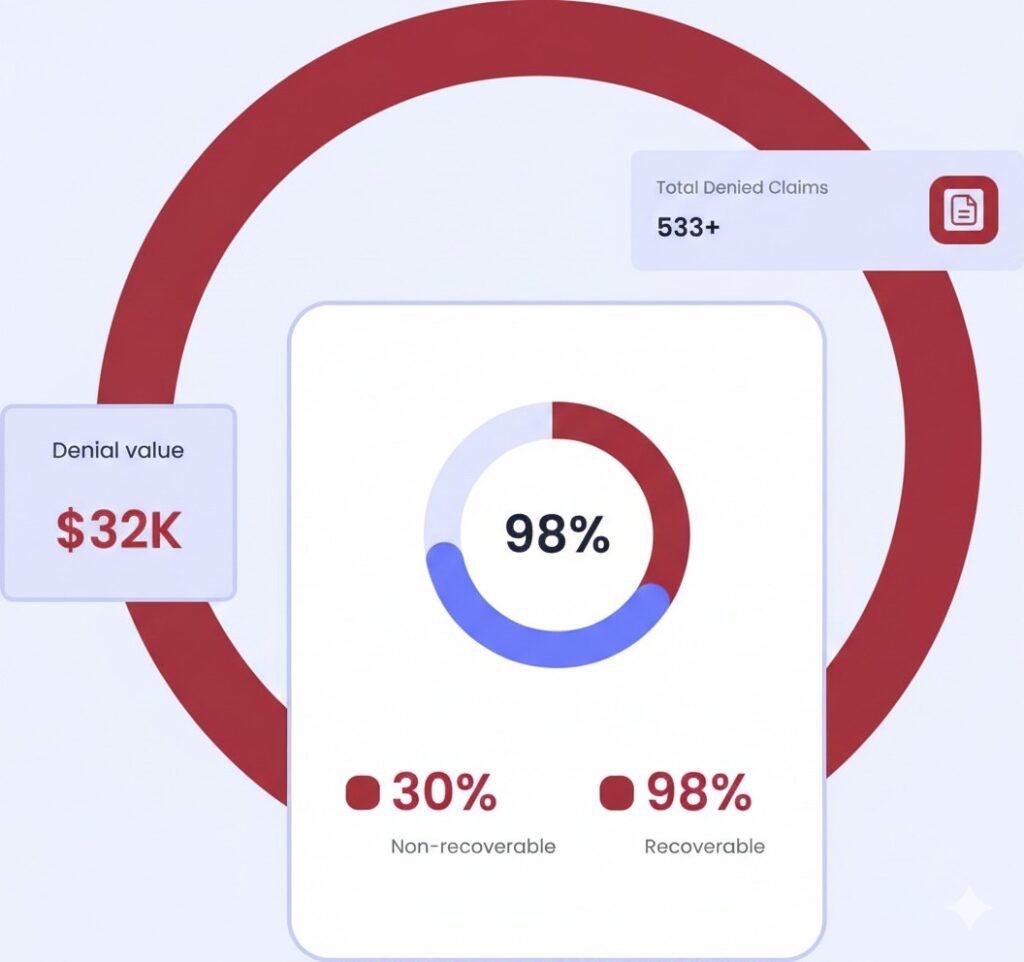

4 Scalable RCM Models that Fit Perfectly For your Practice!
Choose from 4 scalable RCM models to boost profitability, efficiency & get 4 free tailored quotes. Grow your practice by choosing the right revenue cycle management services that are profitable and efficient.
Testimonials
What Our Clients Say
Trusted by 300+ Verified Practices
I would like to send out a heartfelt appreciation for all of your hard work in helping my Health Counselling clinic take care of our billing and credentialing needs. You have made my job as a practice owner much easier.
